Building Cure and Seattle Children’s Therapeutics are devoted to developing innovative therapies for childhood disease. Meet the first patient to receive a cell therapy treatment produced at Building Cure. When Building Cure opened in fall 2019, Meagan Hollingshead and Josh Chittim had more pressing concerns. Their normally energetic 6-month-old daughter Harper was sick, and multiple […]
This past year, as many individuals sought health care through telemedicine, a question formed in Dr. Gina Sequeira’s mind. As the co-director of the Gender Clinic at Seattle Children’s, her mission is to make gender-affirming care accessible for all youth, and so the capabilities of telehealth are rightfully an exciting new territory to explore. With […]
Mercy Haub has wanted to cure cancer since she was 7 years old. “The irony of it all is unbelievable,” she said. Today, at 16 years old, that mission still drives her, but now it hits closer to home, more so than she could have ever imagined. A week before the statewide lockdown went into […]
On Dec. 26, 2018, 18-year-old Hannah Nash, an avid basketball player, was hit in the head while at basketball practice. She initially felt a sharp pain and her head felt foggy. She recalled leaving practice abruptly. The next day, she played in a game, but she didn’t feel like herself. “I played terribly,” Nash said. […]
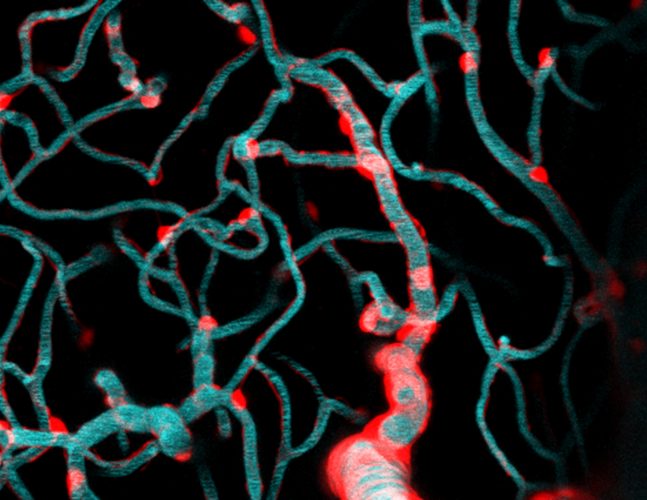
While the human brain has over 400 miles of total vasculature, little is known about the tiny capillaries that make up much of this intricate labyrinth of blood vessels critical for delivering oxygenated blood and nutrients to billions of brain cells. According to Dr. Andy Shih, a principal investigator in the Center for Developmental Biology […]
The U.S. Food and Drug Administration on Feb. 5 approved Bristol Myers Squibb’s Breyanzi, a chimeric antigen receptor (CAR) T-cell therapy used to treat adults with certain types of large B-cell lymphoma who have not responded to or who have relapsed after standard treatments. The approval was supported by research at Seattle Children’s, including the […]
Doctors at Seattle Children’s are investigating whether a simple liquid biopsy containing a small amount of fluid from a patient may someday provide an easier route to a genetic diagnosis in children with vascular or lymphatic malformations. The work is a collaborative effort led by Dr. James Bennett, a clinical geneticist and co-director of the […]
For close to a decade the labs of Dr. David Rawlings at Seattle Children’s Research Institute and Dr. Marion Pepper at the University of Washington have collaborated on a project studying the immune response in malaria infections. As the COVID-19 pandemic gripped the U.S., they turned their expertise and the techniques pioneered for malaria to […]
This year has been filled with unprecedented challenges – physically, mentally, financially – and families are looking forward to putting 2020 behind them. As we collectively usher in a new year, it’s an opportune time to think about small changes we can make to better children’s health in 2021. Dr. Pooja Tandon, a researcher in […]
Before his first breath, Colton Iverson had already received the gift of a lifetime. Just days old, he became the youngest patient to go on a drug recently approved by the U.S. Food and Drug Administration (FDA) for the treatment of a life-threatening genetic condition called very long-chain acyl-CoA dehydrogenase, or VLCAD, deficiency. For his […]