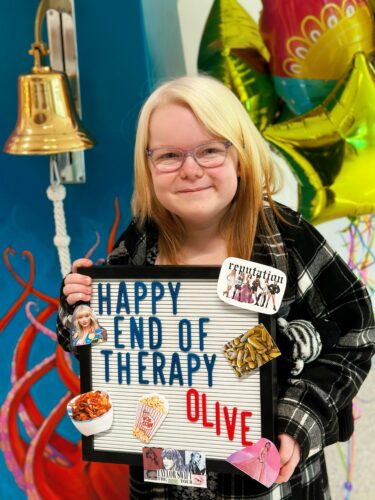
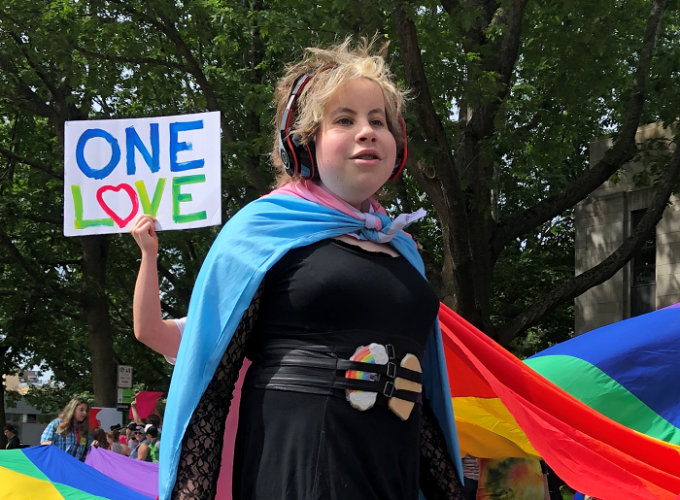Kind and sassy Olive Ray is a typical fifth grader, with a deep love for Taylor Swift, horses, chocolate ice cream, and her little sister, January. But the 10-year-old also has some special skills, like having fun even while getting chemotherapy, raising thousands of dollars for brain tumor research and explaining how clinical trials work […]
In August 2020, just after her third birthday, Aisley began to experience concerning symptoms: headaches in the back of her head, a lack of appetite and vomiting. After a visit to her pediatrician, Aisley was sent to Seattle Children’s for an urgent neurology visit, where she passed the exam with “flying colors,” showing no signs of trouble. Still, Dr. […]
Attention Deficit Hyperactivity Disorder (ADHD) is one of the most common neurodevelopmental disorders that affect children. While patients may first be diagnosed in childhood, ADHD often persists and can be diagnosed at any age. Management of the condition varies as symptoms manifest differently through various milestones in a person’s life. Common ADHD symptoms include trouble […]
Stage was born three weeks premature and soon began having seizures. He was diagnosed with mitochondrial myopathy, a life-threatening diagnosis with no cure and which causes significant muscular and neurological problems. For Stage and his family, it meant unexpected, lifelong care. “I was naïve enough to think that insurance covered everything if your kid was […]
After a family trip to Finland last summer, Jasmine’s family became increasingly concerned about some unusual symptoms she was experiencing. What started as occasional numbness in her lip or left side of her face last spring had progressed to twitching, which the family later learned were increasingly strong seizures. Her family had been proactive in […]
It’s been 12 years, but Brandy Epling still chokes up at the traumatic memory of her firstborn’s birth. It was a difficult pregnancy, with preterm labor forcing a 33-day stay at a southwest Washington hospital for the mom-to-be, followed by months of bedrest. Ultrasounds revealed the baby’s brain was a bit bigger on the left […]
When Jiana was born in August 2021, she appeared to be a typical, healthy newborn baby. “I still remember her pediatrician called her a textbook baby,” recalled Latika, Jiana’s mom. Unfortunately, that normalcy was short lived. On her first day home from the hospital, Jiana’s parents noticed their daughter was twitching. “We were first-time parents […]
March is Cerebral Palsy Awareness Month. Cerebral palsy is a condition that causes differences in how someone moves and controls their muscles. The differences are caused by an injury to a child’s developing brain. The brain injury can happen before, during or after birth. The injury does not change (it is non-progressive), but the effects […]
Update – February 27, 2020: It is our pleasure to share that the individual featured in this story now uses she/her pronouns and goes by the name Iris. She continues to be seen at Seattle Children’s Gender Clinic and advocate for gender affirming healthcare. In celebration of LGBTQ+ Pride Month, On the Pulse shares a […]
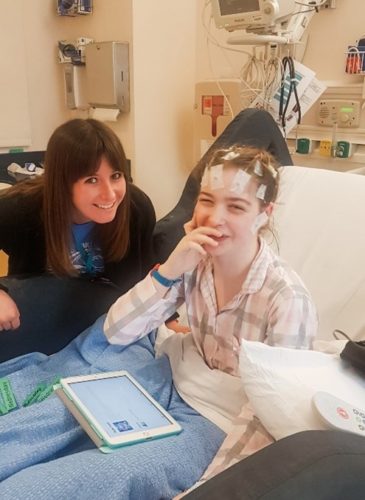
A cutting-edge procedure for epilepsy at Seattle Children’s, known as responsive neurostimulation (RNS), is offering hope and seizure reduction relief to some patients who are still looking for solutions after exploring other treatment options. With RNS, a battery-powered device is placed in a patient’s skull to reduce seizures. A neurosurgeon connects thin wires from the […]