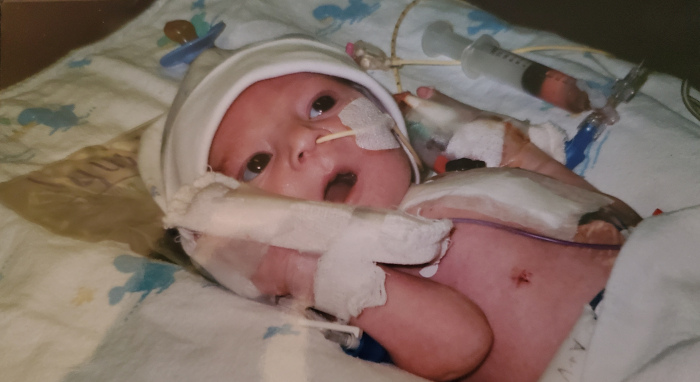
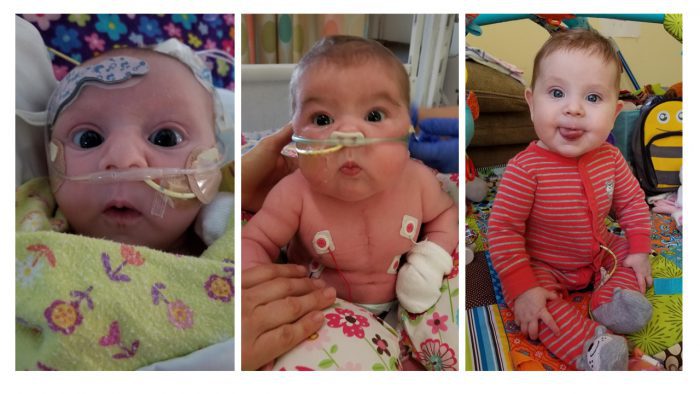
Tuesdays are 2-year-old Malachi Stohr’s favorite days. Every Tuesday, rain or shine, Whitney Stohr and Malachi bundle up and wave to the garbage men as they empty the garbage bins at the end of the driveway. Malachi and Whitney then take a walk around the neighborhood, following the big green truck along its route. Malachi […]
On May 7, 2018, Whitney Stohr slumped to the ground in the corner of her son’s room in Seattle Children’s Pediatric Intensive Care Unit. Her son Malachi, who was born with a severe form of spina bifida, had undergone a tracheostomy days before. When he woke up after the procedure, his pain was so intense […]
Although children don’t typically fall seriously ill from the new coronavirus, doctors in Europe are now expressing concern that children with COVID-19 have developed mysterious symptoms that mimic those appearing with Kawasaki disease. On the Pulse asked Dr. Michael Portman, pediatric cardiologist and director of the Kawasaki Disease Clinic at Seattle Children’s, to help break […]
Worry flooded Candice Andrews’ mind as doctors wheeled her newborn son away for open heart surgery. “I knew about his heart condition since I was 7 months pregnant,” Andrews said. “However, it was still very scary knowing that someone was going to do surgery on my 7-day old baby.” Andrews’ son, Marcus, was born with […]
On July 10, 2018, Avery Crawford entered the world – a beautiful and seemingly perfect baby girl. Little did anyone know about the battle that was secretly raging in her tiny body as her heart struggled to do its job. Avery was a miracle to her parents, Elaine and Jordan Crawford. Their 7-year-old son, Quincy, […]
Just two days before he got sick, Adrian Peterson was practicing martial arts – a typical activity for the active 17-year-old who regularly biked, climbed and hiked. But that all changed in October 2018, when Adrian woke up feeling congested and nauseous. “That was the only forewarning I got for what was to come,” Adrian […]
Mya Garcia, 13, has three birthdays. The first one celebrates the day she came into the world. The other two commemorate the days she was brought back to life. When she turns 18 years old, her mother, Jamie Gonzalez, has a special gift for her miraculous daughter – a heartfelt letter to honor a day […]
A year ago, baby Titus Sickles was fighting for his life. In need of a new heart, doctors didn’t know if he was going to make it to transplant. Patiently and desperately, the family waited on the transplant list, watching as their newborn baby’s heart failed before their eyes. “I knew he wasn’t doing good,” […]
In honor of National Kawasaki Disease Awareness Day on January 26, we are sharing the story of Olivia, a 9-year-old who lives with the disease. Research at Seattle Children’s aims to improve life for children with this condition who are at risk for aneurysms. When Olivia Nelson was 3 years old, her parents noticed that […]
Carolina Castañeda and Jesus Farias were driving home from a family outing with Olivia, their newborn daughter, when they heard her making a strange noise. As first-time parents, they thought it might be normal. However, when Olivia continued making the sound, the couple began to worry. They stopped the car, took Olivia out of the […]