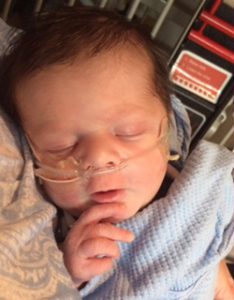
In the early morning hours of May 3, Taylor and Scott Ray welcomed baby Liam into the world at a hospital on Andersen Air Force Base in Guam where they were stationed. After Scott noticed Liam looked a little blue and was breathing heavy, doctors took Liam to get a chest X-ray. Expecting a perfectly […]
A year ago, On the Pulse shared the harrowing story of 8-month-old Lincoln Seay. Lincoln was born with heterotaxy syndrome, a severe birth defect that caused his heart to develop on the opposite side of his body. In order to survive, he needed a heart transplant. In November of last year, Lincoln was placed on […]
Nearly 90% of kids in the U.S. consume too much sodium, putting them at risk for high blood pressure in childhood, and heart disease and stroke later in life. While everyone needs a small amount of sodium to help control the fluid balance in the body and allow nerves and muscles work, too much sodium […]
Babies who need heart surgery in the U.S. have access to advanced healthcare and doctors that get them into the operating room quickly, allowing them to fix problems early and give the babies a chance at healthy growth. But in developing countries, babies wait longer for surgery for a variety of reasons: Fewer qualified doctors, […]
In February 2010, Jennica Clasby knew something was wrong when her 3-year-old daughter, Brooklyn, said she needed to sit down because her “heart hurt.” “I thought it was really odd to hear that coming from a 3-year-old,” Clasby said. “I sat her down on my lap, put my hand over her heart and I was […]
Some parents feed infants and children soy formula and products because they believe they are a healthy alternative to dairy, especially if a child is lactose intolerant. But new research published in the journal Nutrition Research shows that high soy consumption in infants and young children leads to an increased risk of Kawasaki Disease, an […]
Isabella (Bella) Anderson, 18, was running out of time. Her heart was failing and doctors didn’t know how much more it could withstand. She needed a change in luck and some good news. Finally, Bella got just that: a surprise and the news she’d been waiting for. A long road to transplant At only 10 […]
At only 8 months old, Lincoln Seay, has spent the majority of his short life inside the walls of hospitals. This week, however, marks the start of a new chapter: he is finally going home, or at least he’s one step closer to his home back in Alaska. Only 21 days after receiving a life-saving […]
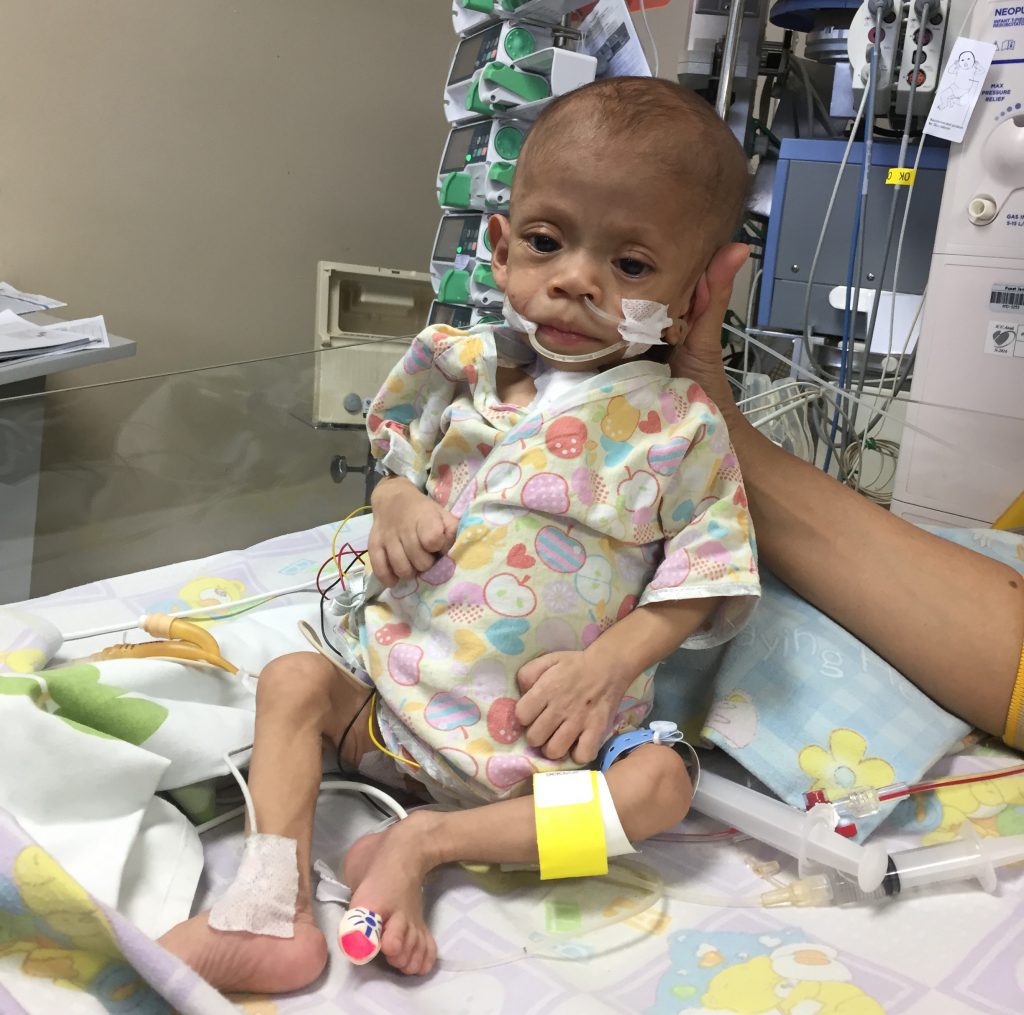
Just shy of his third birthday, little Bowen Warren has already lived up to his name, which literally means “little warrior, small victorious one.” He’s had to overcome a lot in his short life, and that journey has been as his name would suggest: a battle. In February of 2013, Emily Warren was 29 weeks […]
In honor of American Heart Month, On The Pulse asked Dr. Jason Deen, a cardiologist at Seattle Children’s, to provide tips for families who want to make heart-healthy choices. Deen works with families who have children who were born with heart problems, and also cares for families who have children who are obese, most of […]