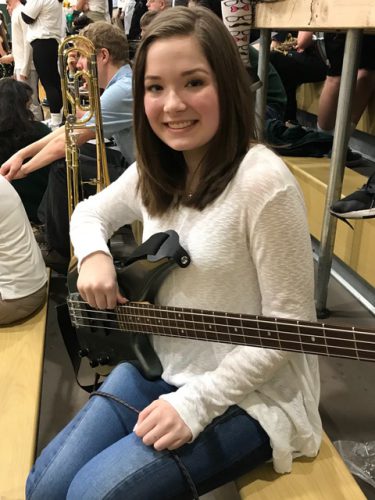More than five years ago, when Dr. Lisa Maves, a scientist at Seattle Children’s Research Institute, first started using CRISPR to make genetic alterations in zebrafish, she saw the potential for the minnow-sized fish to help doctors understand how genetic mutations contribute to a child’s condition. “Essentially, we set out to make a patient’s fish,” […]
Although Katarina Anja, or “Katja,” De Groot was born with a rare heart defect called truncus arteriosus, the active toddler never let her condition stop her from running, playing and going to the park. However, when she was 2 years old, Katja began sleeping for most of the day and withdrawing from the activities she […]
Last month, 6-year-old Hannah Mae Campbell wanted to invite her entire kindergarten class to her birthday party. However, Hannah decided that she couldn’t possibly keep all of the gifts herself; rather she told her mother that she wanted to give them to kids at Seattle Children’s. She said she wanted to give kids something to […]
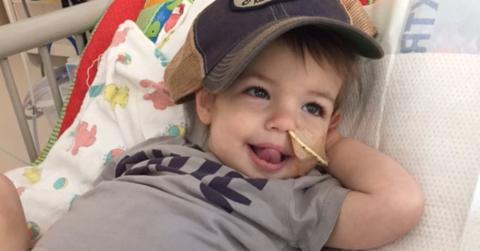
At only 3 months old, Titus Sickles was brought back to life. Today, his family says they have a second birthday to celebrate: the day his new heart started beating for the first time. “He’s a completely new baby,” said Rena Sickles, Titus’ mother. “He has a second chance at life now.” In dire need […]
Whether she’s performing in her school’s jazz band, teaching cello, painting or working as a YMCA counselor, Audrey Wright, 16, seems to do it all. She especially doesn’t let an aneurysm in her heart that developed as a result of Kawasaki disease get in the way of being a busy teenager and her dreams of […]
As she watched her daughter being wheeled into the operating room, a striking memory overcame the flood of anxious thoughts going through Marisela Barragan’s mind. “Just a few months before the heart surgery, my daughter Shanae was telling me how desperately she wanted to try out for her school’s volleyball team,” said Barragan. “Her doctors […]
Rachael Satake holds a 3D-printed replica of her son’s heart condition in her hands during a recent appointment at Seattle Children’s Heart Center. For the first time since learning about the defect midway through pregnancy, she clearly sees how the surgeries he has undergone are helping his heart work despite having only one ventricle. Her […]
Leigh Sturges recalls the day she and her husband, Zach Sturges, learned they were having twins. Seven weeks into their first pregnancy, the Bozeman, Montana, family entered a state of happy shock. “We couldn’t believe it when heard two heart beats on the ultrasound,” she said. “We were realistic about the challenges ahead, deciding it […]
Sara Chenault and her husband, Ed Lang, held their 15-month-old baby, Casey Lang, tightly as they sat outside the hospital on a warm sunny day in July. Casey giggled as he watched the wild rabbits hop through the grass. His eyes lit up and he squealed as he reached for the basketball his dad gently […]
Josie came to Seattle Children’ Emergency Department when she was 2 months old after acquiring a virus and going into respiratory distress. She was also in the beginning stages of heart failure. Statistically, she was lucky to have made it that far. Before birth, Josie was diagnosed with Trisomy 18, a life-threatening condition caused by […]