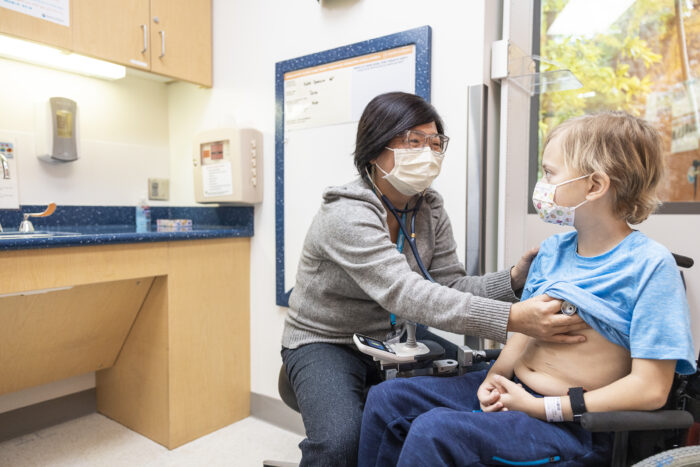
Active kids enjoy improved mental wellness and reduce their risk of heart disease. While the days are short and the weather is often cold or dreary, kids still need to be getting physical activity each and every day. February is American Heart Month and On The Pulse asked Dr. Monique Burton, medical director of the […]
For American Heart Month, Seattle Children’s providers share their tips for helping kids and teens build strong, healthy hearts. Protect young athletes with pre-sport heart screenings Generally, kids are safe to play sports and exercise without concern for cardiac events, but with all types of sports, it is important to do a physical with family history […]
What do you think of when someone says, “hospital food” — green Jell-O anyone? You probably don’t think of create-your-own omelets, barbecued chicken salads, street tacos or hand-tossed pizzas. Hospital food has traditionally gotten a bad rap — and for many years it was deserved. When Gina Sadowski, director of Nutrition, Culinary and Retail, started […]
Can a child’s neighborhood affect his or her weight status, diet, and activity level? According to new research published today in Obesity, the answer is yes. Dr. Brian Saelens, a principal investigator at Seattle Children’s Research Institute who led the study, said children living in neighborhoods with favorable nutrition and activity environments, meaning the neighborhoods […]
The school year has begun, the days are getting shorter and the holidays are right around the corner. As a result, families are on the go in less daylight and variable weather, by foot, bicycles and vehicles. It’s a good time to think about how to use active transportation while staying safe in an increasingly […]
The path to healthier living for children could be the same one they take to school. Children who participated in adult-supervised group bicycle rides to and from school increased their moderate-to-vigorous physical activity by 21 minutes per day and daily cycling commutes by 45%, according to a pilot study recently published in the American Journal […]
Nearly 90% of kids in the U.S. consume too much sodium, putting them at risk for high blood pressure in childhood, and heart disease and stroke later in life. While everyone needs a small amount of sodium to help control the fluid balance in the body and allow nerves and muscles work, too much sodium […]
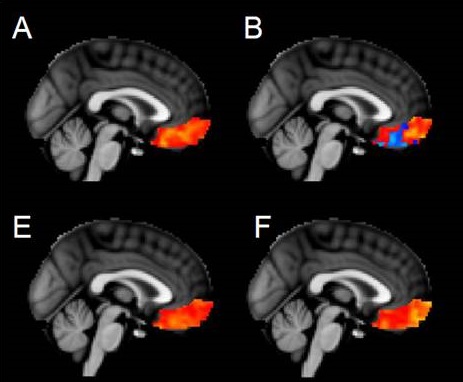
Are brain signals in obese children different than brain signals in normal weight children? Researchers at Seattle Children’s hope to answer that question with a new trial that uses magnetic resonance imaging (MRI) to study brain signaling in children ages 9-11. Dr. Christian Roth, a pediatric endocrinologist and researcher at Seattle Children’s Research Institute, is […]
Traditional advice for helping families ensure their children and teens maintain a healthy weight begins with a focus on balancing calories consumed from food and beverages with calories used through physical activity and growth. Dr. Lenna Liu, a pediatrician at Seattle Children’s Odessa Brown Children’s Clinic and Child Wellness Clinic, uses a slightly different approach […]
Dr. Anisa Ibrahim was 6 in 1993 when her family came to Seattle from Somalia, driven from their country by civil war. In the beginning, everything about their new country was exciting and confusing — especially the supermarket. “We were used to going to the market every day to buy fresh food,” recalls Ibrahim, now […]