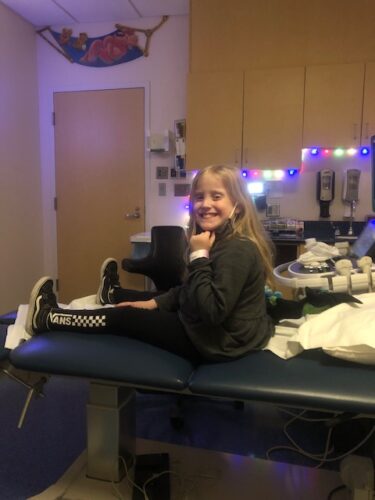
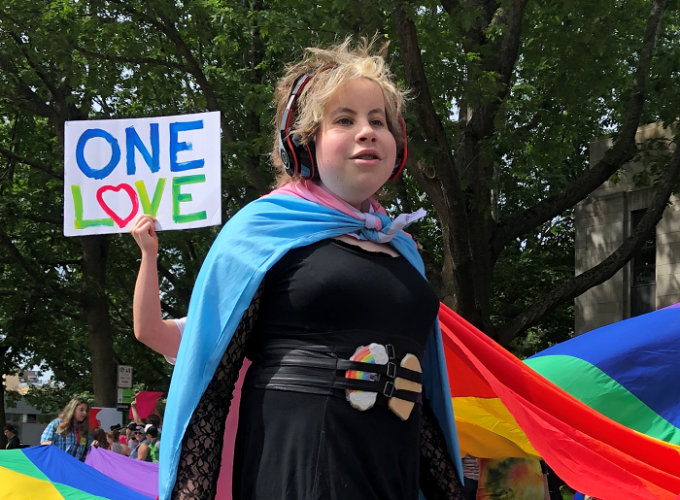PART ONE: From witnessing exceptional care and compassion given to children in their own lives, to receiving treatment first-hand, this weekly series features Seattle Children’s employees and the life experiences that drove them to pursue careers in healthcare. Shortly after Sofia Carlo finished the sixth grade, she started experiencing bouts of intense back pain. “I […]
On the Pulse
As smoky air covers large portions of Western Washington due to of wildfires, many parents wonder what they can do to keep their kids protected. Breathing in wildfire smoke is unhealthy for everyone, however children are at extra risk for negative health effects. Infants and children under age 18, whose lungs and airways are still […]
Seattle Children’s is thrilled to welcome Jamie Phillips as its senior vice president and chief operating officer (COO). As a leader with over 25 years of healthcare administration experience, Phillips comes onboard with both an exceptional resume and a genuine desire to serve and make a difference for Seattle Children’s patients, families and workforce.
Since 2015, Renton-based Wizards of the Coast, a family of studios specializing in role-playing, trading card and digital games, has participated in Extra Life, a fundraising program of Children’s Miracle Network Hospitals. Extra Life brings together tabletop and video gamers to raise money for member children’s hospitals across North America. Funds raised through Wizards’ Secret Lair […]
Katie and Nic Harmston were distraught as they drove to Kaiser for an ultrasound in July 2021. Katie was six and a half weeks pregnant but was experiencing symptoms of a miscarriage. They both feared the worst. The Harmstons held their breath as the ultrasound began. After a moment, the sonographer smiled and said, […]
Across the country, children both young and old are preparing to celebrate another evening of Halloween, filled with costumes, activities, sweet treats and fun with friends. In fact, in 2021 alone, over 42 million kids between the ages of 5 and 14 went trick-or-treating, according to the latest data compiled by the U.S. Census Bureau. […]
Update – February 27, 2020: It is our pleasure to share that the individual featured in this story now uses she/her pronouns and goes by the name Iris. She continues to be seen at Seattle Children’s Gender Clinic and advocate for gender affirming healthcare. In celebration of LGBTQ+ Pride Month, On the Pulse shares a […]
After receiving a life-saving liver transplant at Seattle Children’s, 4-year-old Ruby Josephine Mwamba is thriving and living a dramatically different life than she was at this time last year. Ruby was born with biliary atresia, a liver condition that occurs when a baby’s bile ducts do not form normally and are unable drain bile. Bile […]
Researchers at the Centers for Disease Control and Prevention (CDC) have teamed up with clinicians at Seattle Children’s to identify and evaluate the best urologic management for newborns and young children with spina bifida in a nationwide study called (Urologic Management to Preserve Initial REnal function (UMPIRE). Launched in 2014, the multi-site, multi-year UMPIRE program […]
With each new school year often comes new questions for many parents about their child’s health. For children with health conditions, understanding when and how to best communicate with teachers and school staff about a child’s medical needs, determining the proper amount of information to disclose, and identifying the right programs and services for students […]