At Seattle Children’s, many children and young adults with cancer are finding hope in T-cell immunotherapy – an experimental treatment that boosts a patient’s immune system and uses it to fight a disease. Seattle Children’s researchers are leading clinical trials in which a patient’s T cells are reprogrammed to express a chimeric antigen receptor (CAR) […]
When asked about the birth of her daughter Harper, Sydney Beare lights up. “Harper was 8 pounds, 1 ounce, 21.5 inches and the most beautiful baby I’ve ever seen!” she said. By all accounts, Harper was an exceptionally happy, and seemingly healthy, baby. She began sleeping though the night when she was just a few […]
April Merrill is a 6-year-old who loves to sing and dance. Yet, her struggle with an anxiety disorder called selective mutism hinders her ability to do the activities that showcase her vibrant and joyful personality. “Her voice disappears, as April describes it,” said Kelly Merrill, April’s mother. “She said that she wants to talk but […]
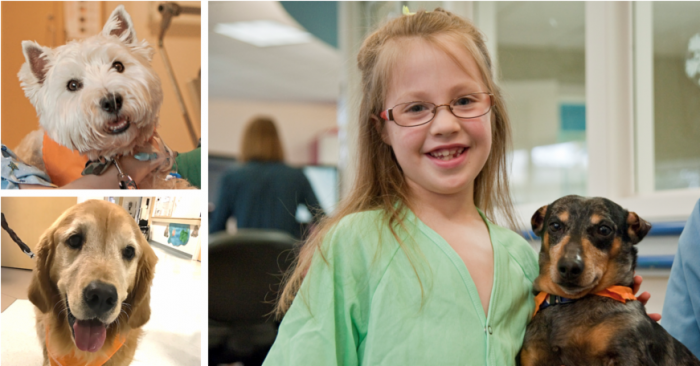
In honor of National Dog Day, On the Pulse is recognizing three unique four-legged visitors who bring joy to kids at Seattle Children’s. When a child is in need of some cheering up during a hospital stay, Seattle Children’s knows just the right MVP for the task – Most Valuable Pup that is. With their […]
In 2009, during Laurina Barker’s 20-week ultrasound, she and her husband Ryan received news that no expecting parents want to hear. “The technician turned to me and said something looked different and that they would have my doctor call me,” said Barker. A couple of days later, the Barkers would learn their baby had congenital […]
When 4-year-old Sho Hansen entered the doors of Seattle Children’s Bellevue Clinic and Surgery Center to get his tonsils removed, he clung on tightly to his mother. “After his name was called and we sat in the exam room, all he wanted to do was sit in my lap and not acknowledge anyone that came […]
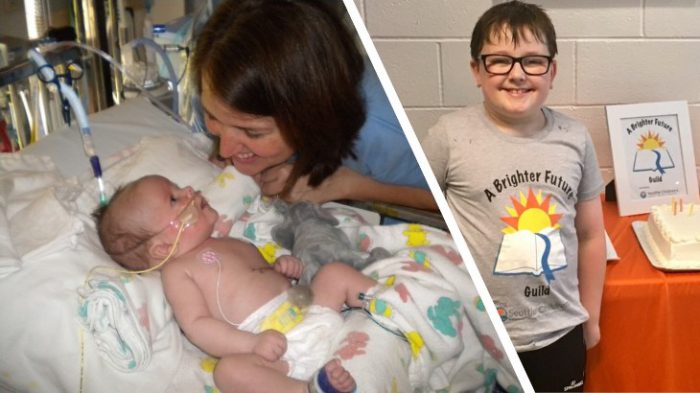
A newborn boy was admitted to Seattle Children’s Neonatal Intensive Care Unit (NICU) earlier this year with arthrogryposis — a condition where an infant cannot move, their joints becoming frozen in place. When geneticist Dr. Jimmy Bennett met the infant, he was on a respirator and could only move his eyes. “We didn’t know the […]
Claire and Emma Brennan are 13-year-olds who are always on-the-run. Whether it’s sprinting across the basketball court or flying to their next volleyball tournament halfway across the country, these twin sisters stop at nothing to achieve athletic excellence. “Claire and Emma have sports practice almost every day of the week,” said their mother, Cathy Brennan. […]
Last month, 6-year-old Hannah Mae Campbell wanted to invite her entire kindergarten class to her birthday party. However, Hannah decided that she couldn’t possibly keep all of the gifts herself; rather she told her mother that she wanted to give them to kids at Seattle Children’s. She said she wanted to give kids something to […]
There is a tremendous need for improved access to mental health care and resources for children and teens nationwide. At Seattle Children’s, its commitment to helping address this need spans not only within the Seattle community, but throughout the region. According to the U.S. Centers for Disease Control and Prevention, nearly 1 in 5 children […]